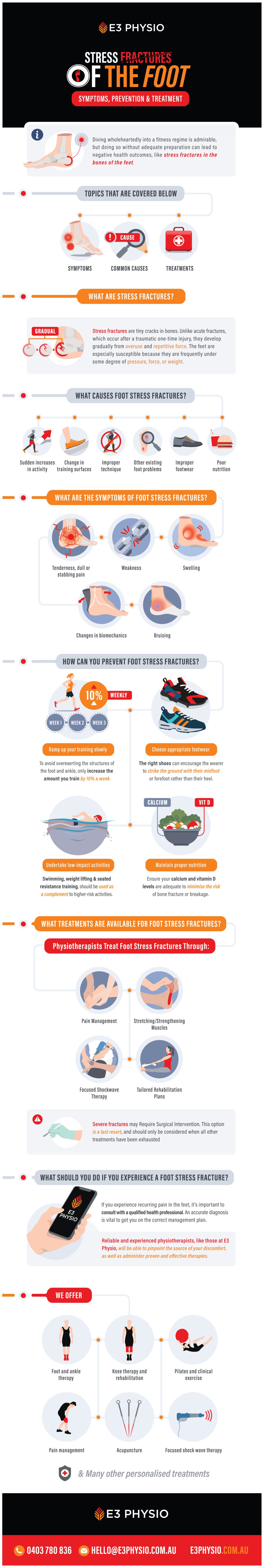
How to Relieve Sciatic Nerve Pain
With up to 40% of people experiencing some form of the condition in their lifetime, sciatica is a significant health concern. The good news is that it doesn’t have to be. Through conservative treatment and appropriate preventative measures, it’s possible to manage and relieve sciatic pain safely and effectively.

What is Sciatica?
Sciatica refers to shooting, burning, or ‘electric’ pain that originates in the lower back and runs down the back of the leg (typically only one, though it occasionally affects both). Sudden movements, and sitting or standing for extended periods may make this pain more severe.
It results from irritation or injury to the sciatic nerve – the thickest and longest nerve in the human body. Stemming from five individual roots in the lower spinal column, it travels down the back of each leg before splitting into smaller nerves just below the knee.
In more severe cases, along with the pain described above, people often report muscle weakness in the affected leg and foot, a ‘pins and needles’ sensation along the limb, and numbness (1).
What Causes Sciatica?
While there are countless potential risk factors for sciatica, these are some of the more common:
Manual Labour
Predisposition to sciatica has been shown amongst workers in physically demanding roles, including machine operators, truck drivers, and others that perform repetitive, awkward movements (2).
Poor Movement Patterns
Poor movement patterns can place additional strain on the lower back, particularly during strenuous activities such as weight training.
Inactivity
Sitting for extended periods can result in a raft of negative health outcomes, including weight gain and a lack of muscular development. These heighten the risk for developing sciatica.
Previous Injury
An injury to your lower spine or the muscles of the back means you’re more likely to suffer from sciatica in the future.
Age
With age comes natural wear and tear of the tissues and disks of the spine. Such changes leave your nerves more prone to being irritated or injured.
E3 Physio’s Catherine Ketsimur runs through one of the simplest ways to prevent sciatic nerve pain.
What Treatments are Available for Sciatica Pain?
Physiotherapy
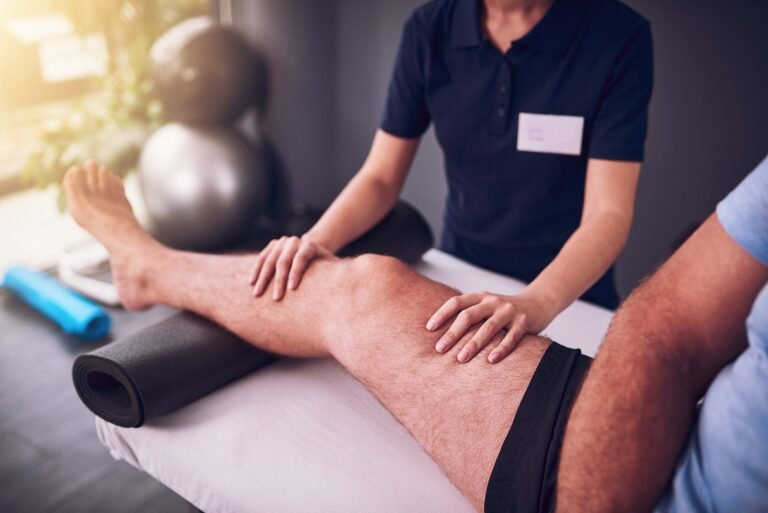
Physiotherapy is all that’s needed to effectively manage most cases of sciatica. It typically centres around stretching and strengthening the muscles of the core (i.e. the abdomen and back) in order to release pressure on the nerve, improve posture, and mitigate harmful movement patterns.
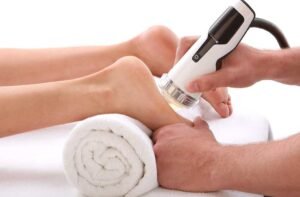
A number of pain management techniques may be employed to make this process more achievable for the patient. These include acupuncture, focused shockwave therapy, massage, and joint mobilisation.
After treating any acute pain and instructing the patient on beneficial movements in-clinic, the physiotherapist can then develop a tailored exercise plan that provides long-term relief. These are often a mix of at-home exercises and stretches, as well as aerobic workouts such as swimming, water aerobics, and walking.
At E3 Physio, we offer pilates and clinical exercise sessions that are perfect for safely strengthening the core and improving mobility.
Steroid Injections
In cases that are not resolving, the GP may consider corticosteroid injections. These are administered directly into the lower back and may provide up to three months relief from sciatica, though their continued use is associated with a number of serious side effects, some of which are irreversible (3).
Medication
Your doctor may prescribe anti-inflammatory or muscle relaxant medication to help ease the pain of sciatica in the short term.
Surgery
Reserved only for cases involving severe or enduring symptoms (like loss of bowel or bladder control, enduring pain, and significant weakness), surgery involves removing bone spurs or the portion of the herniated disk responsible for the compressed sciatic nerve (4).
What Should You do if You Experience Sciatica Pain?
If you experience sciatica, it’s important to consult with a qualified health professional. An accurate diagnosis is vital to get you on the correct management plan as there are many causes for pain down the back of the leg. Reliable and experienced physiotherapists, like those at E3 Physio, will be able to pinpoint the source of your discomfort, and administer proven and effective therapies.
At E3, we help patients manage sciatica through a combination of pain relief and active stretching and strengthening treatments. This multifaceted approach has allowed countless clients to overcome this intrusive pain and return to doing the things they love.
You can reach out to our friendly team via phone, or book an appointment online.